 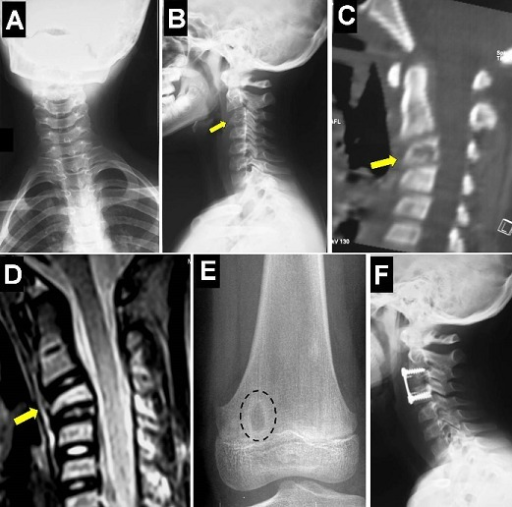
No obvious bone fusion was found on CT 1 year after surgery, so we plan to conduct careful follow-up. 1, 10 Although revision surgery was required because of postoperative surgical site infection, substantial improvement in neurological symptoms was observed 1 year after surgery. 2 Approximately 40% of all patients with Down syndrome who undergo cervical spine surgery have perioperative complications, and approximately 30% require revision surgery. Orthopedic surgery for patients with Down syndrome is known to be associated with an increased risk of surgical site infection and bone union failure. To our knowledge, this 27-month-old boy is the youngest patient with Down syndrome to undergo posterior occipitoaxial fixation. 14, 15 The present case shows that intraoperative 3D CT image–guided navigation with an O-arm scanner was useful for inserting screws into very thin pedicles. There are few reports of surgical treatment for upper cervical instability in patients younger than 3 years old with skeletal dysplasia due to chondrodysplasia and posttraumatic instability. 10, 13 Surgical treatment for upper cervical instability in skeletal dysplasia is challenging, especially in very young pediatric patients because of their small and fragile musculoskeletal structures. The mean age of the patients was 13.2 years, and the youngest patient was 3.8 years old. 
11, 12 The present case highlights that upper cervical instability due to Down syndrome may cause rapid spinal cord injury.Ī recent systematic review and meta-analysis of surgical correction of atlantoaxial instability in patients with Down syndrome indicated that a total of 149 patients with Down syndrome and atlantoaxial instability treated with upper cervical fusion have been reported. Radiographic studies have been conducted to evaluate the instability of the upper cervical spine in young patients with Down syndrome and to predict the appearance of future symptoms, but no consensus has yet been obtained. 1–3 In the present case, emergency surgery was inevitable. Although very rare, the instability can rapidly lead to respiratory dysfunction and dysphagia because of spinal cord disorders, which can cause sudden death. 1, 10 Atlantoaxial instability is a common cause of cervical pain, torticollis, and neurological dysfunction. Postoperative surgical site infection and insufficient decompression with reduction of atlantoaxial instability occurred, and revision surgery was required however, a good clinical outcome and bone fusion were observed 1 year after surgery.ĭespite the reported 15% incidence of upper cervical (craniocervical and atlantoaxial) instability in Down syndrome, symptomatic upper cervical instability has been described to occur in as little as 1%–2% of individuals with Down syndrome. It is very rare and challenging to demonstrate cervical spine fusion in pediatric patients younger than 3 years old, and, to our knowledge, this 27-month-old patient represents the youngest case in a patient with Down syndrome. It warns that Down syndrome in the very young pediatric population may lead to rapid progression of spinal cord injury and life crisis. There are several clinical implications of the present case. Therefore, no posterior arch resection was performed in the first operation. The first surgery was performed urgently because of progressive respiratory dysfunction the priority was to prevent the progression of exacerbation safely by reduction of the C1 ring and stabilizing C1–2 as much as possible. The halo vest was removed postoperatively with the patient under general anesthesia, and a postoperative radiographic image was obtained ( Fig. A plate with rods was placed (Synapse 4.0 Occipito-Cervico-Thoracic Fixation System, DePuy Synthes) along with artificial bone (Grafton, Medtronic). Pedicle and occipital screws were placed at C5, C7, and T2 (3.5-mm diameter, 5-mm length) using intraoperative 3D CT image–guided navigation with an O-arm scanner as previously described 7–9 ( Fig. Additionally, we decided that the anchorage of each screw was not good because of poor bone quality, and it was necessary to extend the anchor to the level of T2 to obtain sufficient stability to support the weight of the head. However, his pedicles were very thin, and we could not find pedicles in the upper cervical spine into which a pedicle screw could be inserted. Ten scalp pins were inserted by probing with the fingers ( Fig. The patient was fitted with a halo vest (Lil’ Angel Halo, Össur) under general anesthesia and placed prone on a Jackson table (Mizuho OSI). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
